Lipedema (also called Lipoedema) is a chronic medical condition characterized by an abnormal accumulation of fat cells, primarily in the legs, buttocks, and occasionally in the arms.
This condition predominantly affects women and is often misdiagnosed as simple obesity or lymphedema. Lipedema is also distinguished by its symmetrical (bilateral) presentation and the disproportion between upper and lower body growth over time.
Lipoedema was first identified in the 1940s at the Mayo Clinic by Dr. Edgar Allen and his colleagues. Their pioneering research highlighted this under-recognized condition, distinguishing it from simple obesity and lymphedema.
Despite this early identification, awareness and understanding of lipoedema in the medical community have been limited, resulting in many patients remaining undiagnosed or misdiagnosed for extended periods.
Lipedema is a complex and misunderstood condition requiring greater awareness and a compassionate approach to diagnosis and management. Proper understanding and early intervention can significantly enhance the quality of life for those affected, minimizing the physical and emotional toll of this chronic disease.
How Common is Lipedema?
Prevalence and Statistics
Estimating the precise prevalence of lipedema is challenging due to underdiagnosis or misdiagnosis as obesity or lymphedema. However, studies suggest that lipedema may affect up to 11% of the female population worldwide. The condition is rarely diagnosed in men, with female-to-male reports suggesting ratios as high as 100:1, largely due to hormonal influences.
Demographic Data
Age:
Lipedema can onset at any age but typically becomes evident during puberty, pregnancy, or menopause – periods characterized by significant hormonal changes. While the condition can develop in adolescence, initial symptoms are often dismissed as normal weight gain.
Gender:
Lipedema predominantly affects women, with very few documented cases in men. The strong link to female hormonal cycles and patterns highlights the potential influence of estrogen.
Global Distribution and Variations
Lipedema has been documented worldwide, affecting individuals across various ethnicities and regions. However, awareness and diagnosis rates vary substantially from one country to another, influenced by healthcare practices, practitioner awareness, and cultural perceptions of body weight and shape. Countries with more advanced research in the field, such as Germany and the United States, tend to report higher diagnosis rates, though this may also reflect higher awareness levels rather than a genuine increased prevalence.
Lipedema is more common than many realize, affecting a significant portion of the female population across the globe. Its onset is closely linked to hormonal changes, making it a critical condition to recognize for those working with women’s health. While global distribution is widespread, the rate of diagnosis vastly differs, calling for increased awareness and educational efforts worldwide to ensure those affected by lipedema receive the support and treatment they need.
Types of Lipedema
See body areas covered in red.
Lipedema manifests in different body regions and is categorized into various types based on its primary location. Understanding these types can help in early diagnosis and appropriate treatment. Here are the main types of lipedema:
Type I: Buttocks and Hips
In Type I lipedema, the abnormal fat distribution primarily affects the buttocks and hips.
Characteristics
- Fat concentration around the pelvis region.
- Noticeable roundness and enlargement of the buttocks.
- Relatively unaffected thighs and legs.
Impact
- Difficulty finding well-fitting clothes for the lower body.
- Increased pressure on the hips can lead to pain and limited mobility.
Type II: Thighs and Upper Legs
Type II lipedema focuses on the upper legs, including the area from the buttocks to the knees.
Characteristics
- Fat deposits more prominently in the thighs.
- Skin texture may become uneven, with dimpling (resembling cellulite).
- Disproportion between the upper and lower body.
Impact
- Restricted range of motion due to fat accumulation around the knee.
- High propensity for bruising and tenderness in the thigh region.
Type III: Calves
In Type III lipedema, the calves are the main area of fat accumulation, extending from the knee down to the ankles.
Characteristics
- Significant swelling of the calves.
- Minimal fat deposition in the thighs or upper legs.
- Cankles (blending of calves and ankles due to swelling and fat).
Impact
- Difficulty in walking or engaging in physical activities.
- High sensitivity and bruising in the lower legs.
Type IV: Arms
Type IV lipedema affects the arms, a less common but equally debilitating variation.
Characteristics
- Fat build-up from the shoulders to the wrists.
- Symmetrical swelling on both arms.
- Minimal to no involvement of lower extremities.
Impact
- Challenges in performing daily activities requiring arm movement.
- Increased risk of arm discomfort and reduced mobility.
Type V: Lower Legs
Type V lipedema is marked by fat accumulation below the knees, including the ankles and lower legs.
Characteristics
- Prominent swelling in the lower legs.
- Reduced fat in the upper legs and thighs.
- Heavy and congested feeling in the feet and ankles.
Impact
- Significant pain and swelling, making standing or walking for long periods difficult.
- Frequent misdiagnosis as venous issues or other conditions affecting lower legs.
Each type of lipedema has its own unique impact on body structure and daily life, highlighting the necessity for tailored diagnosis and treatment. Recognizing these specific types helps medical professionals provide better care and support for those affected by this chronic condition. Through increased awareness and understanding, we can improve the quality of life for individuals living with different types of lipedema.
What are the Usual Complications of Lipedema?
Lipedema can lead to several complications, which can be categorized into physical complications, psychological impacts, and associated health conditions.
Physical Complications
- Mobility Issues:
- The disproportionate fat distribution and swelling can cause significant mobility challenges.
- Difficulty in walking or engaging in daily activities is common, leading to a sedentary lifestyle.
- Pain:
- Individuals with lipedema often experience pain, tenderness, and a feeling of heaviness in the affected areas.
- The pain can be chronic, severely impacting quality of life.
Psychological Impact
- Self-Esteem:
- The cosmetic appearance of lipedema can lead to body image issues.
- Many individuals suffer from low self-esteem and social anxiety due to their appearance.
- Depression:
- The chronic nature of the condition and its physical manifestations can lead to feelings of hopelessness and depression.
- The psychological burden can be as debilitating as the physical symptoms.
Associated Health Conditions
- Lymphedema:
- Lipedema can lead to secondary lymphedema, where excessive fluid accumulates in the tissues, causing further swelling and discomfort.
- The combination of lipedema and lymphedema, known as lipo-lymphedema, exacerbates mobility issues and pain.
- Obesity:
- While not all individuals with lipedema are obese, there is a higher prevalence of obesity among those with the condition.
- Weight gain can worsen lipedema symptoms, creating a vicious cycle.
Symptoms of Lipoedema/Lipedema
Lipedema, often misspelled as lipoedema, is a chronic condition involving the abnormal accumulation of fat, predominantly in the lower extremities. Understanding its symptoms is crucial for early diagnosis and management.
Early Signs and Symptoms
- Symmetrical Fat Accumulation:
- Lipedema often begins with a noticeable and symmetrical increase in fat in the legs, hips, buttocks, and sometimes arms.
- The feet and hands are usually spared, leading to a distinct ledge where the fat stops.
- Pain and Tenderness:
- Individuals may experience pain or tenderness in the affected areas.
- The skin may feel softer and cooler to the touch.
- Easy Bruising:
- Affected areas bruise easily due to increased fragility of blood vessels.
- Bruises may appear without any significant trauma.
- Swelling that Doesn’t Respond to Elevation or Diuretics:
- Unlike common edema, swelling in lipedema does not improve with leg elevation or diuretic medications.
Progression and Worsening Signs
- Increased Swelling and Heaviness:
- Over time, swelling and a feeling of heaviness in the affected areas may worsen, especially with prolonged standing or sitting.
- Mobility Issues:
- The progressive nature of lipedema can lead to difficulties in mobility and an increase in sedentary behavior.
- Walking and physical activities become more challenging.
- Hardening of Tissues (Fibrosis):
- As lipedema progresses, the fat can become firmer due to fibrosis (scar tissue formation).
- This can lead to stiffness and reduced flexibility.
- Psychological Impact:
- Chronic pain, cosmetic concerns, and mobility issues can contribute to depression, anxiety, and social withdrawal.
Distinguishing Lipedema from Other Conditions
- Lipedema vs. Obesity:
- While obesity affects fat distribution all over the body, lipedema primarily affects the lower extremities and often has a distinct demarcation where the fat stops.
- People with lipedema may have a disproportionately smaller waist relative to the legs.
- Lipedema vs. Lymphedema:
- Lymphedema is characterized by the accumulation of lymph fluid, usually affecting one limb and involving the hands or feet, unlike lipedema.
- Lipedema-related swelling does not respond to diuretics or leg elevation as lymphedema might.
- Lipedema vs. Cellulite:
- Cellulite is a cosmetic condition caused by fat pushing against connective tissue under the skin, creating a dimpled appearance and is usually not painful.
- Lipedema involves painful, symmetrical fatty deposits that can lead to significant health concerns if left untreated.
Recognizing the symptoms of lipedema early can lead to better management and improved quality of life. If you suspect you have lipedema, consult a healthcare professional for a suitable diagnosis and treatment plan.
Causes of Lipedema
Lipedema is a complex and poorly understood condition involving the abnormal accumulation of fat, primarily in the lower extremities. Although the exact cause of lipedema remains unclear, research points to a combination of genetic, hormonal, and environmental factors.
Genetic Factors
- Family History:
- Lipedema often runs in families, suggesting a strong genetic component.
- Individuals with a family history of the condition are at a higher risk of developing it themselves.
- Inherited Traits:
- Certain genetic markers and mutations may predispose individuals to lipedema.
- Research is ongoing to identify specific genes involved in the condition.
Hormonal Influences
- Hormonal Changes:
- Lipedema typically manifests or worsens at times of significant hormonal changes such as puberty, pregnancy, and menopause.
- This suggests that female hormones, particularly estrogen, may play a key role in the development and progression of the condition.
- Sex Predisposition:
- Lipedema predominantly affects women, with very few cases reported in men, further indicating the influence of female hormonal factors.
Environmental Triggers
- Lifestyle Factors:
- Although lifestyle factors alone do not cause lipedema, certain elements such as diet and physical activity levels can influence its severity.
- A sedentary lifestyle and poor diet may exacerbate symptoms, while healthy habits may help manage them.
- Trauma:
- There is some evidence to suggest that physical trauma, surgery, or significant weight gain can trigger or worsen the manifestation of lipedema.
Current Research and Hypotheses
- Microvascular Dysfunction:
- One leading hypothesis is that lipedema involves microvascular dysfunction, affecting the small blood vessels and capillaries in the affected areas.
- This dysfunction may lead to increased permeability of blood vessels, causing fat cells to accumulate abnormally.
- Inflammatory Processes:
- Research indicates that chronic inflammation may be a contributing factor.
- Higher levels of inflammatory markers have been found in individuals with lipedema, suggesting a potential link.
- Adipose Tissue Abnormalities:
- Studies are also investigating abnormalities in the adipose (fat) tissue itself, including altered cell function and signaling pathways.
- These abnormalities may lead to the characteristic enlargement and painfulness of fatty tissues seen in lipedema.
While the exact causes of lipedema are still being studied, it is clear that the condition results from a multifactorial interplay of genetic, hormonal, and environmental factors. Ongoing research continues to explore these aspects to better understand and eventually develop targeted treatments for lipedema.
Diagnosis and Tests of Lipedema
Clinical Assessment Methods
Diagnosing lipedema begins with a thorough clinical assessment by a healthcare professional. This involves:
- Physical Examination:
- The doctor will physically examine the affected areas, often the legs and arms, noting any swelling, tenderness, or abnormal fat distribution.
- They will check for the classic signs of lipedema, such as symmetry in the swelling and whether it stops at the ankles and wrists.
- Medical Imaging:
- Advanced imaging techniques like ultrasound or MRI can help distinguish lipedema from other conditions like lymphedema or obesity. These tools offer a detailed view of tissue composition and fluid accumulation.
- Pain and Tenderness Assessment:
- The healthcare provider will ask about your pain levels and tenderness in swollen areas. Pain in fatty areas can be a telling symptom of lipedema.
Role of Patient History
A comprehensive patient history is crucial for an accurate lipedema diagnosis. Important aspects include:
- Family History:
- Lipedema often runs in families, so noting any relatives with similar symptoms is important.
- Onset and Progression:
- Patients will be asked when they first noticed the symptoms and whether they have worsened over time. Lipedema typically starts or worsens around times of hormonal change such as puberty, pregnancy, or menopause.
- Previous Treatments:
- Documenting any previous attempts to treat the swelling, such as diet, exercise, or diuretics, and their effectiveness can help differentiate lipedema from other conditions.
- Associated Symptoms:
- Discuss any other symptoms like easy bruising, fatigue, or frequent infections, which may aid in the diagnosis.
Importance of Early Diagnosis
Early diagnosis of lipedema is vital for several reasons:
- Effective Management:
- Early diagnosis allows for timely intervention, which can significantly slow the progression of the disease and alleviate symptoms.
- Tailored Treatment Plans:
- Identifying the condition early allows for the creation of a personalized treatment plan, which may include specialized therapies, compression garments, and, in some cases, surgical options like liposuction.
- Improved Quality of Life:
- Early treatment can help prevent complications, such as mobility issues, severe pain, and psychological distress, thereby improving the overall quality of life for the patient.
- Avoiding Misdiagnosis:
- Early diagnosis helps prevent misdiagnosis with other conditions like obesity or lymphedema, ensuring that patients receive the correct treatment and support.
Stages of Lipedema
Lipedema is a progressive condition characterized by abnormal fat deposits, primarily in the legs and arms. It is crucial to recognize the different stages of lipedema to manage the condition effectively. Here is an easy-to-read breakdown of the stages of lipedema:
Stage 1 Lipedema: Early, Smooth Skin Texture
In the early stage of lipedema, the skin maintains a smooth texture despite the onset of fat buildup. Characteristics of Stage 1 include:
- Fat Accumulation: There is noticeable fat accumulation in the legs and occasionally in the arms.
- Symmetry: The swelling is symmetrical, meaning both legs or both arms are equally affected.
- Soft Skin: The skin appears soft to the touch and there is no visible change in skin texture.
- No Pain: At this stage, pain and tenderness may be mild or absent.
Key Considerations:
- Early Identification: Recognizing lipedema at this stage can be challenging but is critical for effective management.
- Specialist Consultation: Seeking consultation with a healthcare professional or a specialist like Dr. Salameh can help in early diagnosis.
Stage 2 Lipedema: Uneven Skin Texture
As lipedema progresses to Stage 2, changes in skin texture become more apparent. Characteristics of this stage include:
- Nodules and Lumps: Fat deposits become more nodular and uneven, creating a bumpy or dimpled appearance.
- Increased Swelling: Swelling becomes more pronounced, particularly after prolonged periods of standing or sitting.
- Tenderness: There may be increased pain and tenderness in the affected areas.
- Subcutaneous Fat: The subcutaneous fat layers (just under the skin) become thicker and more noticeable.
Key Considerations:
- Medical Intervention: Early intervention at this stage can prevent worsening symptoms.
- Customized Treatment: Treatments like compression garments and manual lymphatic drainage can help manage symptoms.
Stage 3 Lipedema: Hardening and Fibrosis
In Stage 3 of lipedema, the condition becomes more severe, leading to hardening and fibrosis (formation of excess fibrous connective tissue). Characteristics include:
- Hard Skin: The fat becomes harder and feels more substantial under the skin.
- Excess Tissue: Large, protruding fat deposits may form, often described as “lobular” appearance.
- Skin Changes: The skin may appear rougher and less elastic.
- Mobility Issues: Increased fat deposits and fibrosis can lead to reduced mobility and greater discomfort.
Key Considerations:
- Surgical Options: Surgical interventions like LippyLipo can be considered to remove excessive fat and improve quality of life.
- Ongoing Care: Continuous management with specialized therapies and lifestyle changes is essential.
Stage 4 Lipedema: Advanced Stage with Lymphedema
Stage 4 is the most advanced stage of lipedema, often characterized by the development of secondary lymphedema (venous lymphatic insufficiency). Characteristics include:
- Severe Swelling: Pronounced and severe swelling due to both fat and fluid buildup.
- Lymphedema: The lymphatic system becomes compromised, leading to additional swelling (often referred to as lipo-lymphedema).
- Skin Ulcers: The skin is prone to ulcers and infections due to compromised lymphatic and vascular systems.
- Significant Mobility Issues: Mobility may be severely restricted, impacting daily life and independence.
Key Considerations:
- Comprehensive Care: Intensive medical care, including both surgical and non-surgical treatments, is often necessary.
- Holistic Approach: A multidisciplinary approach involving specialists in plastic surgery, lymphatic therapy, and other relevant fields can provide the best outcomes.
Understanding the stages of lipedema is crucial for early diagnosis and effective treatment. Whether you are in the early or advanced stages, recognizing the symptoms and seeking appropriate medical intervention can significantly improve your quality of life. If you suspect you have lipedema, schedule a consultation with a specialist like Dr. Salameh to explore your options for management and treatment.
Differences Between Lipedema and Lymphedema
Lipedema and lymphedema are both chronic conditions that cause swelling and other symptoms, but they have distinct underlying mechanisms, presentations, and treatments. Understanding these differences can help in effective diagnosis and management. Here’s a comprehensive, but easy-to-read breakdown:
Pathophysiology
Lipedema:
- Definition: A chronic disorder characterized by abnormal and symmetrical fat accumulation, usually in the lower extremities and sometimes the arms.
- Cause: The exact cause is unknown, but it is believed to be genetic and hormonal.
- Tissue Affected: Primarily affects the subcutaneous fat tissue.
- Lymphatic Involvement: The lymphatic system is usually not directly involved in the early stages but may be affected in advanced stages, leading to lipolymphedema.
Lymphedema:
- Definition: A condition characterized by localized fluid retention and tissue swelling caused by a compromised lymphatic system.
- Cause: Can be congenital (primary lymphedema) or acquired (secondary lymphedema) due to surgery, radiation, infection, or trauma.
- Tissue Affected: Involves lymphatic tissue and causes fluid buildup in the interstitial tissues.
- Lymphatic Involvement: Directly affects the lymphatic system, leading to impaired lymph drainage.
Symptoms and Clinical Presentation
Lipedema:
- Symmetrical Swelling: Typically affects both legs or both arms symmetrically.
- Pain and Sensitivity: Patients often experience pain, tenderness, and easy bruising.
- Textured Skin: Early stages feature smooth skin, while advanced stages show nodular, uneven skin.
- Absence of Foot/Hand Swelling: The feet and hands are usually spared unless the condition progresses to lipolymphedema.
- Fat Deposits: Distinct, disproportionate fat accumulation, often described as “column-like” legs or “batwing” arms.
Lymphedema:
- Asymmetrical Swelling: Can affect one limb or one side of the body asymmetrically.
- Heaviness and Restriction: Patients often feel heaviness, tightness, and restricted movement in the affected area.
- Skin Changes: May cause skin thickening, fibrosis, and in advanced cases, a “peau d’orange” texture (orange peel-like).
- Involvement of Extremities: Can affect the hands or feet, causing significant swelling and fluid retention.
- Recurrent Infections: Prone to skin infections and ulcers due to compromised lymphatic drainage.
Treatment Approaches
Lipedema:
- Compression Therapy: Use of compression garments to manage swelling and improve lymphatic flow.
- Manual Lymphatic Drainage (MLD): Specialized massage techniques to stimulate lymph flow and decrease swelling.
- Liposuction: Surgical removal of excess fat, particularly in advanced stages.
- Exercise and Diet: Low-impact exercises and an anti-inflammatory diet to manage symptoms and improve overall health.
- Medications: Pain management and addressing any hormonal imbalances with medical supervision.
Lymphedema:
- Compression Therapy: Use of compression bandaging and garments to reduce swelling and prevent fluid buildup.
- Manual Lymphatic Drainage (MLD): Gentle massage techniques specifically designed to promote lymph drainage.
- Complete Decongestive Therapy (CDT): A comprehensive approach combining MLD, compression therapy, exercise, and skin care.
- Pneumatic Compression Devices: Devices that apply pressure to the limb to encourage lymphatic flow.
- Surgery: In severe cases, surgical options like lymphovenous anastomosis and lymph node transplantation may be considered.
While both lipedema and lymphedema result in swelling and discomfort, they are fundamentally different conditions with unique underlying mechanisms, symptoms, and treatments. Proper diagnosis by a healthcare professional is essential for effective management.
Here’s a detailed blog post if you need more information on their differences: Lipedema vs. Lymphedema.
Differences Between Lipoedema and Other Reasons for Swelling
Swelling can arise from various conditions, and distinguishing between these causes is crucial for accurate diagnosis and treatment. Below, we explore the differences between lipoedema and other common sources of swelling, including edema from heart, liver, or kidney diseases, venous insufficiency, and obesity-related swelling.
Lipoedema/Lipedema
Definition: Lipoedema is a chronic disorder characterized by abnormal, symmetrical fat accumulation, primarily in the lower extremities and sometimes the arms, usually affecting women.
Key Features:
- Symmetry: Swelling occurs symmetrically in legs and/or arms.
- Pain and Sensitivity: Affected areas are often painful, tender, and prone to bruising.
- Sparing of Hands and Feet: Hands and feet are typically not involved unless the condition progresses to lipolymphoedema.
- Diet-Resistant Fat: Fat deposits in lipoedema do not reduce with diet or exercise alone.
Edema from Heart, Liver, or Kidney Diseases
Edema Definition: Generalized swelling caused by the accumulation of excess fluid in tissues due to underlying organ dysfunction.
Heart Failure-Related Edema:
- Symmetry: Often symmetrical and affects lower extremities.
- Association with Other Symptoms: May be accompanied by shortness of breath, fatigue, and exercise intolerance.
- Pitting Edema: Pressing on the swollen area leaves a dent (pitting).
- Bilateral Leg Swelling: Typically worsens by the end of the day or after prolonged standing.
Liver Disease-Related Edema:
- Abdominal Ascites: Fluid accumulation in the abdominal cavity (ascites) is common.
- Peripheral Edema: Swelling in legs and sometimes the scrotum or abdomen.
- Jaundice: Yellowing of the skin and eyes may be present.
- Pitting Edema: Pressing on the swollen area leaves a dent.
Kidney Disease-Related Edema:
- Generalized Swelling: Can affect the face (especially morning puffiness around the eyes), hands, and legs.
- Proteinuria: Presence of protein in the urine, detectable via urine tests.
- Pitting Edema: Pressing on the swollen area leaves a dent.
Venous Insufficiency
Definition: A condition where the veins struggle to return blood from the legs back to the heart, leading to blood pooling and swelling.
Key Features:
- Asymmetrical or Symmetrical Swelling: Swelling can be either asymmetrical or occur in both legs.
- Heaviness and Pain: Legs feel heavy, achy, and may cramp.
- Skin Changes: Skin may become thick, leathery, and develop a brownish discoloration.
- Varicose Veins: Prominent, swollen veins are often visible.
- Pitting Edema: Pressing on the swollen area leaves a dent.
Obesity-Related Swelling
Definition: Swelling that occurs due to increased body fat and weight, putting pressure on the lymphatic and venous systems.
Key Features:
- Symmetrical Swelling: Generally symmetric, affecting both legs and possibly arms.
- Pressure Induced: Increased pressure on veins and lymphatics from excessive body weight.
- Pitting Edema: May or may not have pitting; skin changes are less pronounced than in venous insufficiency.
- Improvement with Weight Loss: Swelling may decrease with significant weight loss through diet and exercise.
- Generalized Obesity: Overall increased body fat, not localized like in lipoedema.
Read more: Lipedema or Just Fat Legs? Crucial Things to Know
Swelling Comparison Summary Table
Recognizing the differences between lipoedema and other causes of swelling is essential for proper diagnosis and treatment. If you are experiencing persistent or unusual swelling, consult a healthcare professional for an accurate diagnosis and appropriate management plan. Early intervention can often lead to better outcomes and improved quality of life.
Treatment for Lipedema
Lipoedema treatment requires personalized plans to address individual needs.
Usual Treatments for Lipedema
- Dietary Modifications: Adopt a balanced diet to manage symptoms.
- Exercise and Physical Activity: Regular low-impact exercise improves mobility and reduces discomfort.
- Compression Garments: Wearing these can help alleviate pain and prevent further swelling.
- Manual Lymphatic Drainage (MLD): A specialized massage technique to stimulate lymph flow and reduce fluid build-up.
- Vibration Therapy: Utilizes mechanical vibrations to improve circulation and lymphatic drainage.
- Aqua Therapy: Exercising in water eases joint stress and enhances circulation.
- Tumescent Liposuction or Awake Lipo: Minimally invasive procedure that uses a local anesthetic to remove excess fat.
- Water-Assisted Liposuction (WAL): Employs a water jet to dislodge fat cells, making them easier to remove.
- Lipoaspiration Techniques: Various methods to remove fat deposits and improve limb shape.
Each treatment should be tailored to suit the patient’s specific symptoms and overall health conditions.
LippyLipo by Dr. Salameh: Best Lipedema Surgeon in the US
Awake LippyLipo
Awake LippyLipo, developed by Dr. Salameh, is an innovative, minimally invasive liposuction technique designed to reshape and contour the body while the patient remains comfortably awake. This procedure enhances safety, reduces recovery time, and increases patient involvement in the treatment process.
Lippy Lipo Procedure Specifics and Benefits
Awake LippyLipo utilizes advanced techniques to precisely target and remove unwanted fat with minimal discomfort. During the procedure, a local anesthetic is applied, allowing patients to remain awake and communicative, contributing to optimal results. The key benefits include:
- Reduced Risk: Eliminates the risks associated with general anesthesia.
- Quick Recovery: Patients experience less downtime, often resuming normal activities quickly.
- Precision and Control: The awake method allows for real-time adjustments, ensuring a personalized outcome.
- Minimal Scarring: Smaller incisions lead to less scarring and a more natural look.
- Increased Comfort: Many patients report feeling at ease due to the local anesthesia and supportive environment.
Dr. Salameh’s Patients’ LippyLipo Experience and Success Stories
Here are some of our patients’ amazing results:
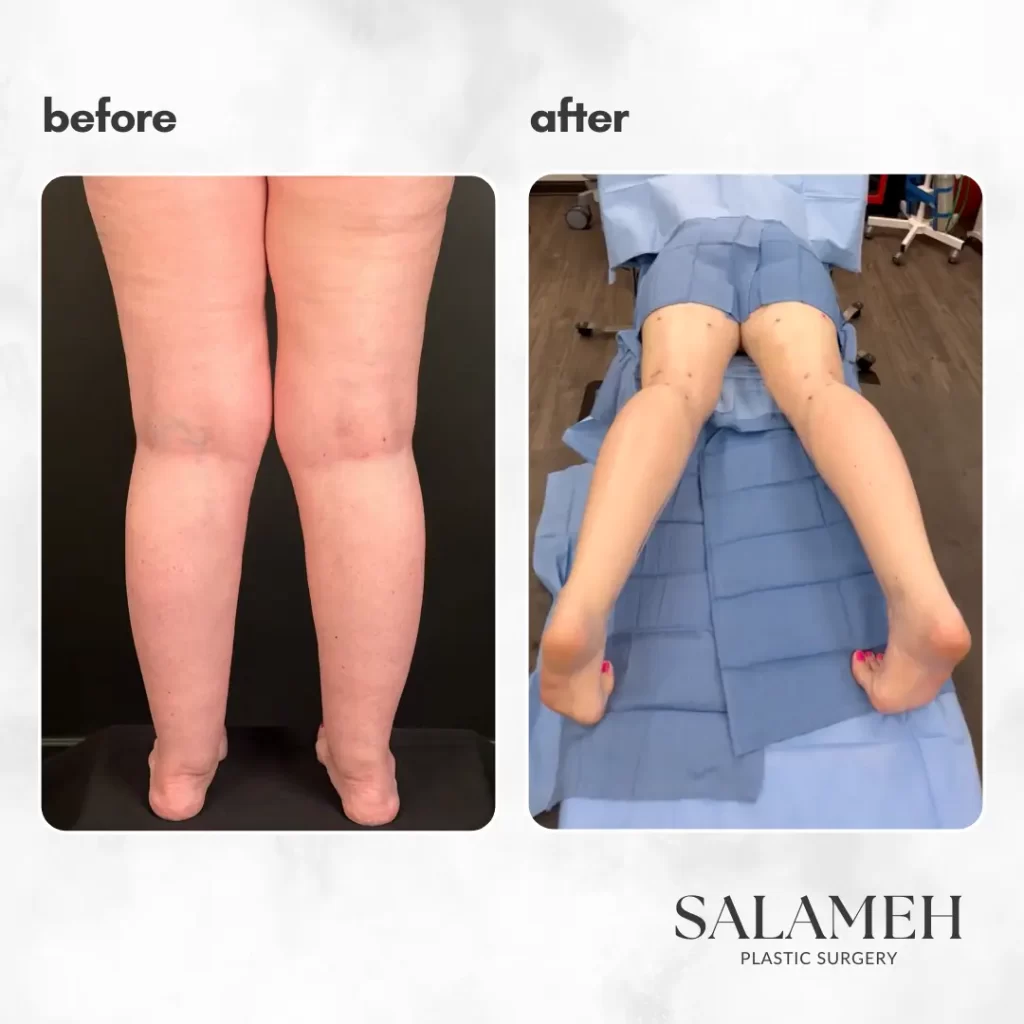
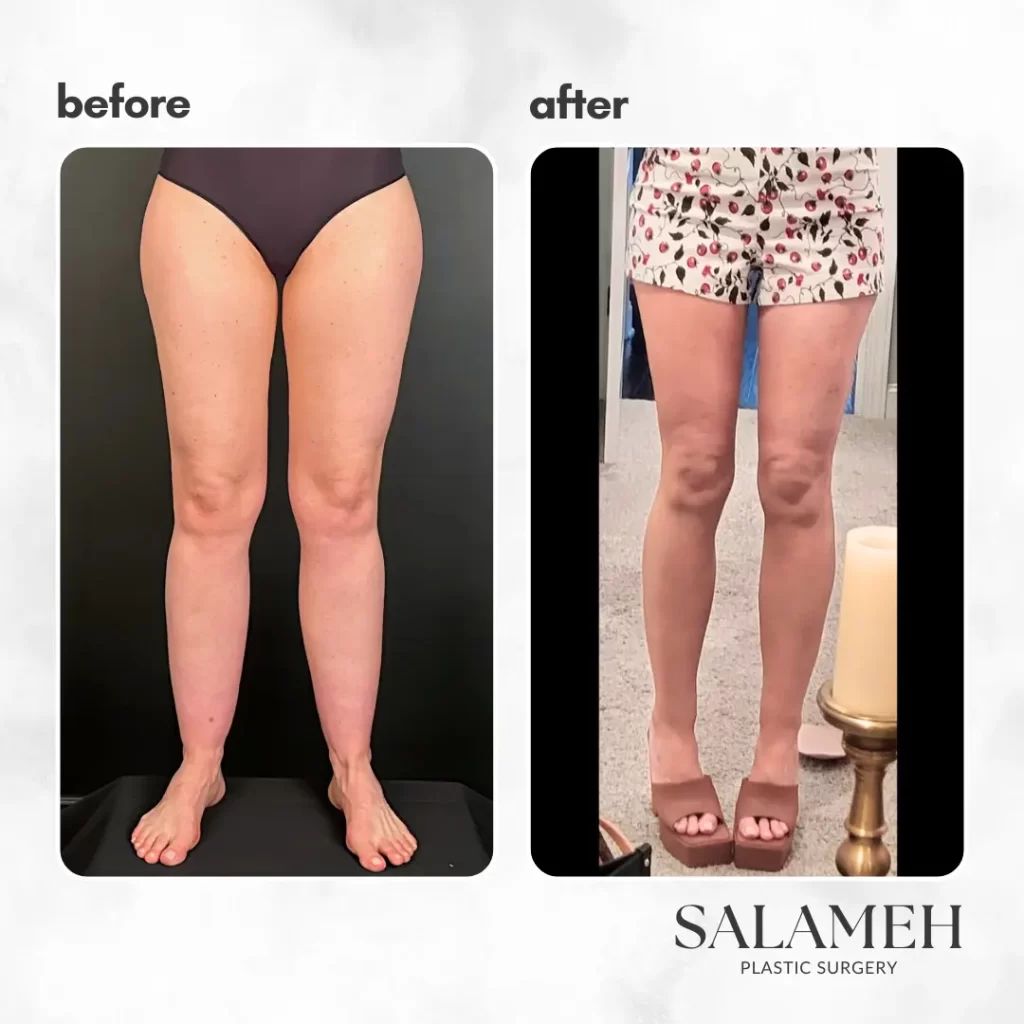
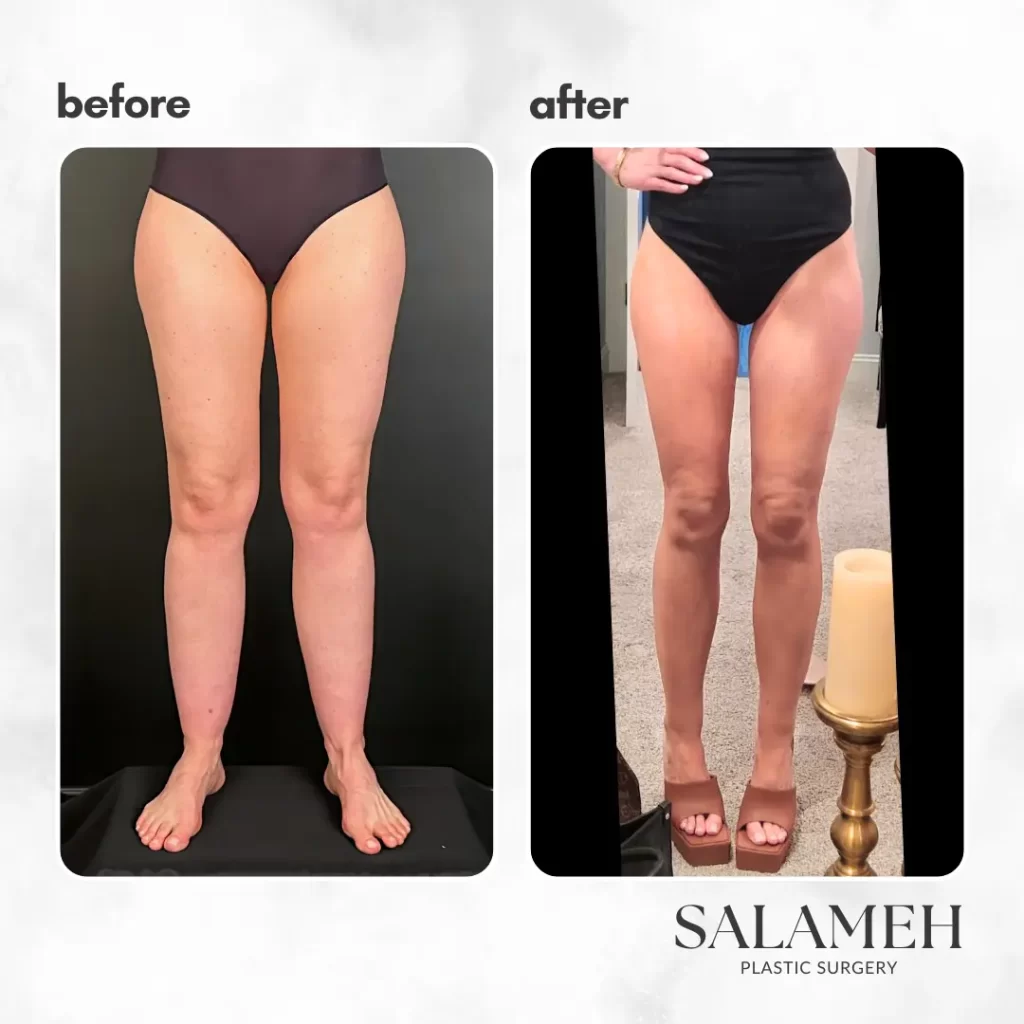
Many patients have shared their positive experiences with Awake LippyLipo:
- Leah’s Journey: Leah wholeheartedly recommends Salameh LippyLipo to anyone looking for experienced lipedema specialist. The center’s dedication to awake liposuction for Lipedema sets them apart from other practices, providing patients like Leah with an innovative and tailored solution. The relationship at the center is built on trust, ensuring that each patient’s emotional well-being is just as important as their physical health.
Read more of Leah’s LippyLipo Experience
- Ally’s Transformation: “Since my surgery on 11/7/2022. I am screaming and crying happy tears. I do NOT have that achy toothache in my legs. I can stand without shifting back and forth. I am not constantly moving my legs. At the end of the night, I do not have that pressure and heaviness. It is GONE!” Ally recalled.
Read more of Ally’s journey and her triumph over lipedema
Importance of Seeking Certified Specialists
When dealing with conditions like Lipoedema, it is essential to consult certified and experienced specialists. Certified providers ensure:
- Expertise: Specialists possess the necessary training and experience to deliver effective treatments.
- Safety: Certified practitioners adhere to the highest safety standards and protocols.
- Personalized Care: Certified specialists are adept at creating individualized treatment plans tailored to your specific needs.
- Up-to-date Practices: They remain informed about the latest medical advancements and techniques.
Prevention of Lipedema
Lifestyle Changes
Adopting a healthy lifestyle can play a significant role in managing and potentially mitigating the effects of Lipedema. Key lifestyle changes include:
- Balanced Diet: Emphasize a diet rich in anti-inflammatory foods such as fruits, vegetables, lean proteins, and omega-3 fatty acids.
- Regular Exercise: Low-impact activities like swimming, walking, and cycling can enhance lymphatic flow and reduce discomfort.
- Weight Management: Maintaining a healthy weight can alleviate symptoms, although it does not outright prevent Lipedema.
- Hydration: Staying well-hydrated supports overall health and can improve skin elasticity.
Early Detection Strategies
Early detection of Lipedema can lead to more effective management and better outcomes. Strategies include:
- Self-Examination: Regularly check for signs of disproportionate fat accumulation, especially in the legs and hips.
- Medical Consultation: Seek medical advice if unusual symptoms arise, such as persistent swelling or pain.
- Family History: Be aware of your family medical history, as Lipedema often has a genetic component.
Preventing Complications
Preventing complications associated with Lipedema involves proactive measures:
- Compression Therapy: Wearing compression garments can reduce swelling and prevent fluid buildup.
- Lymphatic Drainage Massage: Regular massages can promote lymphatic circulation and relieve discomfort.
- Skin Care: Maintain good skin hygiene to prevent infections or ulcerations, which can be common in advanced stages of Lipedema.
How Can I Lower My Risk of Lipedema?
While there is no surefire way to prevent Lipedema, certain steps can help lower your risk:
Genetic Counseling
Given the genetic predisposition of Lipedema, genetic counseling can be beneficial for individuals with a family history of the condition. This can help:
- Assess Risk: Determine the likelihood of developing Lipedema based on your genetic makeup.
- Educate: Provide information on the inheritance patterns and preventative measures.
- Plan Ahead: Make informed decisions regarding lifestyle and health monitoring.
Hormonal Balance
Hormonal imbalances are often implicated in the onset and progression of Lipedema. Maintaining hormonal balance involves:
- Regular Monitoring: Regular blood tests to check hormonal levels.
- Medical Guidance: Consult with endocrinologists to manage conditions like thyroid disorders or PCOS.
- Stress Reduction: Practices like yoga and meditation can help maintain hormonal equilibrium.
Regular Health Check-Ups
Consistent health check-ups are imperative for early detection and management:
- Annual Exams: Routine visits to your healthcare provider for comprehensive evaluations.
- Specialist Consultations: Regular appointments with specialists such as endocrinologists or vascular surgeons.
- Diagnostic Tests: Periodic imaging tests to monitor the progression of Lipedema or detect potential complications.
Lipedema Outlook / Prognosis
Long-Term Health Outcomes
With early detection and effective management, individuals with Lipedema can anticipate the following:
- Improved Quality of Life: Symptom management strategies can significantly enhance daily function.
- Stabilized Condition: While Lipedema is progressive, interventions can slow its advancement.
- Complication Prevention: Ongoing care can prevent severe complications like lymphoedema or infections.
Potential for Symptom Management
Although there is no cure for Lipedema, effective management is achievable through:
- Therapeutic Interventions: Treatments like compression therapy, manual lymph drainage, and liposuction.
- Lifestyle Modifications: Adopting a healthy lifestyle to manage symptoms and improve overall well-being.
- Medical Support: Regular follow-ups with a healthcare team dedicated to managing Lipedema.
Coping with Chronic Conditions
Living with a chronic condition like Lipedema requires a multifaceted approach:
- Emotional Support: Engage with support groups or mental health professionals to navigate the emotional challenges.
- Education and Advocacy: Empower yourself with knowledge and advocate for your needs with healthcare providers.
- Adaptive Strategies: Develop coping mechanisms, such as pacing activities and seeking ergonomic solutions to daily tasks.
By adopting these strategies, individuals with Lipedema can lead fulfilling lives, effectively managing symptoms and reducing the risk of complications.
What Can I Expect if I Have Lipedema?
Daily Living and Adaptations
Living with Lipedema involves various adaptations to manage daily activities comfortably and effectively. Here’s what you can expect:
- Mobility Aids: Some individuals may benefit from using mobility aids such as canes or wheelchairs, depending on their symptoms.
- Clothing Choices: Compression garments are essential for symptom management and can be worn under everyday clothing.
- Ergonomic Adjustments: Make household and workplace adjustments to reduce strain and improve ease of movement.
Social and Emotional Implications
Lipedema often carries social and emotional ramifications:
- Body Image Issues: Dealing with disproportionate body fat can affect body image and self-esteem.
- Social Stigma: Misunderstanding and lack of awareness about Lipedema can lead to social stigma and isolation.
- Support Networks: Building a network of supportive friends, family, and online communities can alleviate feelings of isolation.
Prognosis and Disease Progression
Understanding the prognosis and potential disease progression is crucial:
- Stages of Lipedema: The condition is progressive and generally categorized into stages, each with increasing severity.
- Symptom Evolution: Symptoms like pain, swelling, and bruising can worsen over time if not managed properly.
- Long-term Outlook: With early detection and effective management, the impact of Lipedema can be reduced, and quality of life can be maintained.
Living With Lipedema
Day-to-day Management Tips
Effective day-to-day management can significantly improve your quality of life:
- Consistent Routine: Establish a daily routine that includes skin care, compression garment wear, and exercise.
- Dietary Considerations: Focus on anti-inflammatory foods and maintain a balanced diet to manage symptoms.
- Hydration: Keep hydrated to support lymphatic health and overall well-being.
Navigating Social Situations
Navigating social situations can be challenging but manageable with the right approach:
- Educate Others: Explain Lipedema to friends and colleagues to foster understanding and empathy.
- Comfortable Outings: Choose social activities that accommodate your physical comfort and capabilities.
- Assertiveness: Be assertive about your needs and limitations without feeling guilty or embarrassed.
Mental Health Considerations
Mental health is an integral part of living with Lipedema:
- Therapy and Counseling: Seek professional help to address issues like depression, anxiety, and body image.
- Mind-Body Practices: Engage in activities like yoga, meditation, or mindfulness to reduce stress and enhance emotional well-being.
- Support Groups: Join support groups specific to Lipedema to share experiences and gain emotional support.
How do I Take Care of Myself?
Self-care Routines
Developing self-care routines is crucial for managing Lipedema:
- Skin Care: Regularly moisturize and inspect your skin to prevent infections and complications.
- Massage Therapy: Incorporate manual lymph drainage massages to promote lymphatic circulation.
- Rest and Recovery: Ensure you get adequate rest and sleep to help your body rejuvenate.
Importance of Self-advocacy
Being your own advocate is essential for proper care:
- Medical Advocacy: Communicate effectively with healthcare providers to ensure you receive appropriate treatment.
- Informed Decisions: Stay educated about Lipedema and the latest treatment options to make informed health choices.
- Empowerment: Empower yourself through knowledge, self-care, and by voicing your needs and concerns.
Building a Support System
A strong support system can provide crucial emotional and practical support:
- Family and Friends: Rely on close friends and family members who understand and support your condition.
- Professional Network: Assemble a team of healthcare professionals, including doctors, physical therapists, and mental health counselors.
- Community Engagement: Engage in local or online communities for additional support, resources, and shared experiences.
By understanding what to expect and how to manage Lipedema, you can take proactive steps to enhance your quality of life and navigate the challenges of living with this chronic condition.
When Should I See My Healthcare Provider?
Signs Necessitating a Medical Visit
It’s essential to recognize when to consult your healthcare provider for managing Lipedema or any other health concerns. Key signs include:
- Increased Pain or Discomfort: Escalating levels of pain that disrupt daily activities.
- Swelling: Unusual or persistent swelling that doesn’t subside with rest or compression.
- Skin Changes: New or worsening skin issues such as discoloration, rashes, or ulcers.
- Mobility Issues: Difficulty moving or walking that is not usual for your condition.
- Frequent Bruising: Unexplained bruises that appear more often or heal slower than usual.
Regular Check-up Frequency
Regular consultations with your healthcare provider play a vital role in effective Lipedema management:
- Initial Diagnosis: Frequent visits during the initial diagnosis phase to establish a treatment plan.
- Ongoing Monitoring: Regular check-ups every 3-6 months to monitor the progression and effectiveness of treatments.
- Symptom Tracking: Scheduled appointments if there’s a noticeable change in symptoms, particularly if they worsen.
Pre- and Post-treatment Consultations
Proper planning and follow-up are essential for treatments related to Lipedema:
- Pre-treatment Consultations: Discuss upcoming procedures, treatments, or changes to your healthcare plan:
- Review potential risks and benefits.
- Understand pre-procedure preparations and instructions.
- Post-treatment Follow-ups: Essential for evaluating the effectiveness of a treatment:
- Monitor for any side effects or complications.
- Adjust the treatment plan as needed based on feedback and results.
When Should I Go to the ER?
Emergency Symptoms
Certain symptoms warrant immediate emergency medical attention. Do not hesitate to go to the ER if you experience:
- Severe Pain: Intense, unmanageable pain that doesn’t improve with usual pain management strategies.
- Difficulty Breathing: Any form of respiratory distress or shortness of breath.
- Chest Pain: Sudden, sharp chest pain can indicate serious conditions like heart complications.
- Extreme Swelling: Rapid or excessive swelling, especially if it affects only one side of the body.
- Signs of Infection: Including high fever, chills, red streaks emanating from a wound, or severe skin irritation.
Complications Requiring Immediate Attention
Certain complications of Lipedema or related conditions may require urgent care:
- Deep Vein Thrombosis (DVT) Symptoms: Swelling, pain, and redness, particularly in one leg, that may indicate a blood clot.
- Lymphedema-related Infections: Sudden, painful swelling with warmth and redness, suggesting possible cellulitis.
- Open Sores or Ulcers: Any wounds that become infected or do not heal properly.
- Unexplained Severe Symptoms: Any sudden, unexplainable symptoms like intense weakness, loss of consciousness, or severe dizziness.
By understanding the signs and symptoms that require medical attention, as well as knowing when to seek emergency care, you can ensure timely and appropriate responses to health complications related to Lipedema. Regular communication with healthcare providers and prompt action in emergencies are critical to managing and mitigating the impact of this condition.
What Questions Should I Ask My Doctor to Effectively Manage Lipedema Condition?
When managing a condition like Lipedema or any other health issue, it’s crucial to have open and informative discussions with your healthcare provider. By asking the right questions, you can better understand your condition and participate actively in your care plan. Here are some key questions to consider.
Treatment Options and Recommendations
Understanding your treatment options is essential for making informed decisions. Consider asking:
- What are the available treatment options for my condition?
- Which treatment do you recommend and why?
- Are there any non-invasive treatments available?
- What are the pros and cons of each treatment option?
- Are there any clinical trials or new treatments I should consider?
Expected Outcomes and Potential Risks
Getting a clear picture of what to expect can help you prepare mentally and physically for your treatment journey. Inquire about:
- What are the expected outcomes of the recommended treatment?
- How long will it take to see results?
- What are the potential risks and side effects of each treatment?
- How will this treatment affect my daily life and activities?
- Are there any long-term risks or complications associated with the treatment?
Lifestyle and Dietary Suggestions
Lifestyle and diet can significantly impact health conditions like Lipedema. Ask your doctor for tailored advice:
- Are there specific dietary recommendations I should follow?
- What types of exercise or physical activity are most beneficial for my condition?
- Are there any activities I should avoid?
- How can I manage stress to help with my condition?
- Are there any lifestyle changes that could help alleviate symptoms or improve outcomes?
Additional Questions to Consider
To get a comprehensive understanding of your condition and management strategies, you might also consider these questions:
- How should I monitor my symptoms, and when should I report changes?
- Are there support groups or resources you recommend for individuals with my condition?
- What should I expect during follow-up visits and ongoing monitoring?
- How can I best prepare for upcoming procedures or treatments?
- What is the long-term outlook for my condition with the recommended treatment plan?
By asking these questions, you can ensure that you have all the necessary information to manage your health effectively. Open communication with your doctor is key to developing a successful treatment plan tailored to your specific needs and lifestyle.

